The real-life creation of human-animal hybrids, which is on the verge of going from hypothesis to reality, has been the subject of ongoing debate since the dawn of genetic engineering. But recent advances have made these creatures of dreams (or nightmares) no longer hypothetical, thanks to two major milestones in the world of xenotransplantation: the transfer of living cells, tissues, or organs from one species to another.
In September 2021, the University of Alabama at Birmingham announced the first successful clinical-grade transplant of gene-edited pig kidneys into a human (albeit brain-dead), replacing the recipient’s native kidneys in a display of function. The kidney, which was attached to the leg of a deceased patient maintained on a ventilator, began functioning—making large amounts of urine—in the short experimental window before being terminated after 54 hours. A similar success connecting pig kidneys to two more brain-dead patients was reported just this week from New York University.
The other major milestone was in January 2022, when the world witnessed the first successful pig heart xenotransplantation. David Bennett Sr., a 57-year-old diagnosed with terminal heart disease, received a genetically modified pig heart at the University of Maryland in Baltimore. While the transplanted porcine heart functioned without immediate rejection by Bennett’s body, he died two months later by a cause not yet determined.
But before it becomes too late to put the genie back in the bottle on pig-to-human xenotransplantation, experts say there are many unresolved questions about whether to fully pop this clinical cork. Much of the debate is likely to boil down to safety first, and second, an analysis of the economic and health costs and benefits of these procedures—not only those borne by society but also by doctors, caregivers, and all those thousands of people who are dying and in need of an organ transplant.
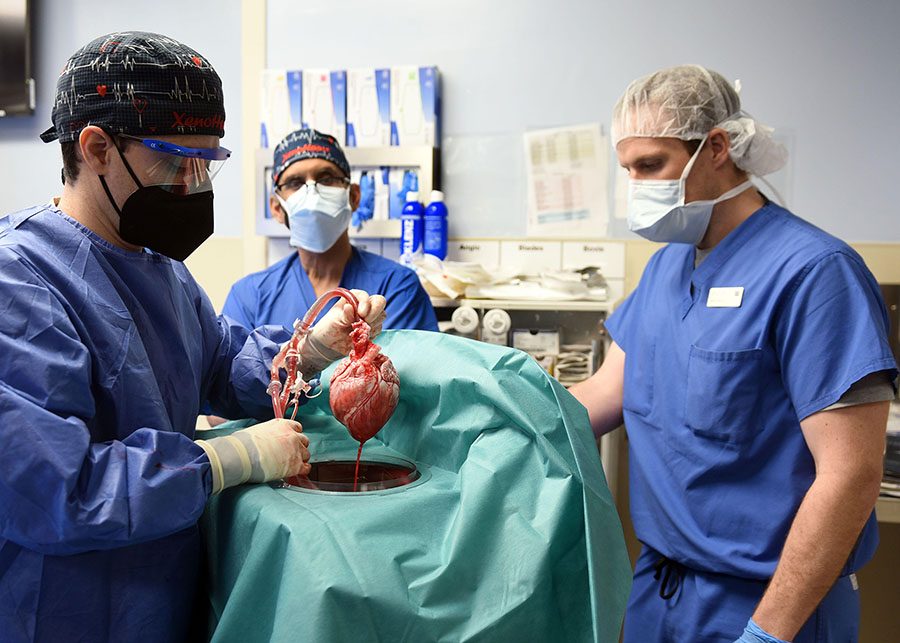
When pigs fly
As it turns out, genetically engineered pig organs actually cost far more than human organs at the moment—a measure of the fact that experimental xenotransplantation animals are grown in carefully controlled settings. Raising genetically engineered pigs in pristine, quarantined, and secure conditions is expensive. The caretakers for the pigs have to wear what are essentially spacesuits to ensure the animals don’t get an infection, and they have to check the pigs frequently to make sure they’re not carrying diseases.
Harvard geneticist George Church points out that the cost of a heart transplant in the United States is around $1.66 million, according to the most recent estimates, while pig transplants, judging solely on the cost of the pig heart transplants for baboons, are a comparative steal at just $500,000. Human organs themselves are cheaper, largely because the organs are donated free of charge by living or deceased donors, but the cost of transplanting a human organ is more expensive because of the cost associated with keeping a deceased donor’s organs viable during transport and flying out transplant surgeons and other experts on a moment’s notice.
But where the financial scales really get upended is when you start to look at transplant waitlists and the cost in human suffering that stems from having such a limited number of donated organs. With pig organ transplants, people may no longer have to wait in an intensive care unit for three months or more, which is the current average wait time for a donor’s heart—or be on dialysis for seven years or more as they wait for a kidney to come available. And the cost in terms of human lives is even greater. Organ waiting lists are long, and they are tragically withering.
According to the Organ Procurement and Transplantation Network, 106,045 men, women, and children are on the national transplant waiting list, but 17 people die each day waiting for an organ (more than 6,000 a year). The vast majority of them are waiting for kidneys; in 2021, there were 90,483 people on the kidney transplant waiting list, but only 24,670 operations were performed. As it turns out, 45 percent of those added to the kidney waiting list are later taken off because they either developed complications, they were no longer deemed eligible, or they simply died waiting.
With a pig, you could potentially have a donor organ whenever you need it.
University of Pittsburgh xenotransplantation researcher and heart transplant surgeon David K.C. Cooper imagines a future day when someone will come to the ER with kidney failure or heart failure: Once their doctors decide they need a transplant, they schedule the surgery for Tuesday morning at nine o’clock, and when they arrive the next day, there will be a fresh, beating pig heart waiting on ice.
“You won’t have to get up in the middle of the night, rent a private jet, and bring the heart back,” Cooper says.
The simple laws of economics suggest that the price of pig organs will drop as availability increases and more companies get into the business of offering porcine tissues. But the financial burden on society could paradoxically grow because the increase in supply of organs would allow more people to get a transplant, increasing total U.S. spending on transplantation medicine.
However, Cooper believes that these financial costs will be offset by savings associated with a reduced need for prolonged pre-operative intensive care, mechanical circulatory support, and human organ retrieval. Referencing a 2016 paper by Philip J. Held from Stanford University Medical School, Cooper points out that the net welfare gain to society from a single viable human kidney is about $1.1 million because kidney recipients would no longer need expensive dialysis treatment, and could in theory get back to work, thus contributing to the economy. Dialysis is not only an inferior treatment for end‐stage renal disease (ESRD), it is also almost 4 times as expensive per quality‐adjusted life‐year (QALY) gained as a transplant recipient. From the viewpoint of society, the net benefit from saving thousands of lives each year and reducing the suffering of 100,000 more receiving dialysis would be about $46 billion per year, with the benefits exceeding the costs by a factor of 3. Accounting for the added surgical costs of more transplants, it would still save taxpayers about $12 billion each year.
It would therefore appear that, if a pig kidney graft function is comparable to a deceased human kidney graft, the cost of the pig kidney will be well worthwhile.
Gone hog wild
But if the economics are relatively straightforward, the ethics of pig-to-human xenotransplantation are much more muddy. This is especially true when it comes to patients’ rights. Since the Nuremberg trials at the end of World War II, it’s been standard practice in the ethics declarations of clinical studies to have some verbiage that a research participant has the right to drop out entirely for any reason at any time. (One notable exception was the Tuskegee Syphilis Study, which had numerous glaring ethical violations, including violating the principle of informed consent, not disclosing diagnoses to patients, and withholding treatment from them.) This puts xenotransplantation between a rock and a hard place because, at least for now, people who elect to take pig organs could not entirely drop out of that clinical trial participation.
“If the recipient acquires a novel zoonotic disease from the pig that could be spread to others, it could become a public health concern.”
According to Rowan University bioethicist Daniel J. Hurst, essentially all regulatory bodies say that people who receive xenotransplant organs have to be monitored for the rest of their lives—not just to ensure their transplanted organ is healthy and their immune system does not reject it but also to ensure they didn’t contract any sort of infection from the pig organ. Such infections could be some emerging, completely unknown porcine endogenous retrovirus (PERV) already present in the pig genome and reactivated into a human infection after the transplant. Or they could be infected with a known animal virus or bacteria fouling the pig organ prior to surgery.
“With xenotransplantation, all the major guidelines state that the xenograft recipient needs to be monitored for the rest of their life with blood draws, imaging, and tissue sampling to ensure they’re still pathogen-free. This is because if the recipient acquires a novel zoonotic disease from the pig that could be spread to others, it could become a public health concern.”
Nobody alive today needs any illustration of the potential societal danger of zoonotic infections—living as we are in the third year of one of the worst animal-derived disease outbreaks in human history. But it’s worth pointing out the extreme infection risk of contaminated pig tissues to transplant recipients because you would essentially be placing the organs in a person’s body and connecting them directly to their bloodstream while giving the people drugs to suppress their immune systems.
The monitoring issue is also a privacy flashpoint, opening up a can of legislative, judiciary, and policy worms. Suppose an organ recipient doesn’t want to participate anymore. Do they have to be forced to do the ongoing testing? What if they get their new pig kidney in Boston and decide that they want to move to rural Montana or overseas, where they may not have the imaging or lab to continue monitoring? Or what if they just don’t show up for their scheduled blood draw?
Matthias Loebe, the chief of heart and lung transplant and mechanical support at the Miami Transplant Institute, says there is very little wiggle room here. “The patient has to make this lifelong commitment to follow up because there’s no option to withdraw from the study,” he says. “They can’t just say that they don’t want to go to their follow-up appointments or be monitored anymore.”
Ironically, Loebe points out, for Bennett, the pig heart recipient, the argument (while repeatedly shot down) was that he was not worthy enough to receive a human heart since he had been convicted of multiple violent crimes. Bennett was acquitted of intent to murder but found guilty of battery and carrying a concealed weapon for the 1988 bar stabbing of Edward Shumaker, condemning the latter to a wheelchair for the rest of his life, which ultimately led to his stroke and premature death. Loebe questioned if such a person would be reliable enough to follow up with lifelong monitoring for diseases that we don’t even know we’re looking for.
Checking our moral math
Julian J. Koplin from Melbourne Law School thinks that the use of these animals requires ethical calculus because there are huge unanswered questions with regard to animal welfare. Pigs are quite socially complex, intelligent creatures, and they are normally raised in pens or pastures with mud to wallow in and fellow pigs to see. But to ensure the safety of their organs, xenotransplant pigs would need to be raised under sterile and isolating conditions to minimize the risks of contracting infectious diseases that could be passed to the recipients. The pig would probably be looking at life in a plastic bubble without any social opportunities—and it’s not going to be a particularly great life, Koplin says. “Xenotransplantation looks much better than factory farming, where the animal would have an unpleasant life and then be killed for a food source. But just because something is less bad than something that’s really bad does not make it alright to do. We have to work through the animal issues seriously and not just wave our hands towards other uses of animals that are currently accepted.”
The real question, as we contemplate how we can save people who would otherwise die for lack of organ transplants, is: Does the moral math check out? Can we calculate the cost-benefit of one human life saved for one animal life used? “All things considered, we will need to weigh out the moral costs and benefits given the current stage of technological development and xenotransplantation,” Koplin says. “Only once you’ve done that analysis it may be possible to justify xenotransplantation.”
There should be a lot of communication between people working on food ethics, animal researchers, and xenotransplantation, he adds. “The same people working up policy for xenotransplantation aren’t the same people drawing up animal welfare guidelines.”
The God squad
While it’s easy to get lost in these ethical and legal conundrums, we must keep an eye out for the ethical benefits. Reflecting on his days running a heart transplant center, Cooper says, “If you have a patient who had a heart transplant and six to eight years later the heart begins to fail, you think, what am I going to do with this patient? If we do nothing, the patient will die. Do we do another transplant? But if this person gets a second transplant, it means somebody’s on the list waiting for their first transplant [who] doesn’t get that transplant and might die.”
With a limited supply of organs well below demand, you have to be very careful to select people who will do very well. “But that will no longer be a problem with the pig transplant,” he says. “You’re not deciding who is the preferable patient to get an organ; now, you’re just giving it to anybody who’s suitable.”
Is it unethical to withhold an organ from someone above a certain age?
Those same ethical issues were seen in the early days of dialysis, which dates back to the 1940s, when there were very few dialysis machines, and committees decided whether people would live or die by selecting which ones should go on dialysis and which ones should not. But as with any zero-sum decision driven by limited resources, there are always people left standing when the music ends. “Let’s say you’ve got this patient who is a brilliant young scientist that might contribute significantly to the world,” postulates Cooper. “Should he go on dialysis, or should this man in his fifties who has four children to support?”
Once transplant surgeries became available, those same quandaries carried over to questions of who gets a donated organ: Is it unethical to withhold an organ from someone above a certain age? What if an organ recipient candidate isn’t a very reliable patient and will not comply with the follow-up procedures? Should we give this organ to somebody who’s a better member of society?
“It’s an almost impossible decision,” Cooper says, adding that in the early days of dialysis the groups tasked with making them were sometimes called God squads because they decided who lives and who dies. “If they decided against you, you would die because you weren’t going to get dialysis.”
That ended with the advent of the Organ Procurement and Transplant Network (OPTN), a public-private partnership operated since the 1980s by the nonprofit United Network of Organ Sharing (UNOS). When an organ becomes available, UNOS creates a list of probable recipients based on blood type, tissue type, organ size, medical urgency, time on the waiting list, and geographical distance between the donor and the receiver and offers the organ to the institution caring for the best-match recipient.
The legend of Cronutt
Xenotransplantation doesn’t need to be limited to the kidney or heart. For example, in some conditions, you could use pig fetal cells to treat neurodegenerative diseases like Alzheimer’s and Parkinson’s, which cost the U.S. nearly $200 billion annually in patient care and lost productivity—a financial burden estimated to increase to $1.1 trillion by 2050.
Putting fetal brain cells from another species into a human may sound outlandish, but this issue is on the horizon. After all, in October 2020, an epileptic sea lion named Cronutt (similar to NYC’s croissant-donut hybrid pastry sensation) underwent an experimental procedure in which researchers injected pig brain cells into his damaged brain. And guess what? Cronutt is alive and well today and back to “normal.”
Unless we’re standing pat with the transplantation status quo or heading towards a Never Let Me Go world where human cloning is implemented on a full scale for the harvesting of vital organs, xenotransplantation is probably coming someday to a clinic near you—so long as it can overcome all the ethical, moral, and legal hurdles along the way.









