No more metal: Living electrodes promise safer, better ways to fix injuries and disease and grow new links between man and machine.
Neurovisionaries dream of one day merging our brains with computers. That era seems closer than ever: Tech pioneers like Elon Musk and Mark Zuckerberg are now pursuing brain implants that aren’t purely for treatment, but could let us do things like communicate telepathically or type with our minds. Others claim we’ll soon have neuroprostheses to enhance our attention and memory, or allow us to integrate our brains with the Internet and control our smart homes with our minds.
Simple electrical implants have been used since the 1980s for deep brain stimulation (DBS), in which wire electrodes penetrating the brain deliver pulses of an electrical current to ease the symptoms of Parkinson’s disease, obsessive-compulsive disorder, and other neurological problems. Rarer, but also in use, are brain implant therapies for people paralyzed by spinal cord injury or other neurological damage. A chip inserted into the brain reads off electrical signals that are translated by a computer to restore some movement and communication. But these brain computer interface (BCI) setups are so complex that they have so far only been used in a few dozen cases.
The truth is, the hardware just isn’t there yet. Implants have major drawbacks. They require surgery to remove a piece of skull. And the metal electrodes that penetrate the brain eventually cause scar tissue to form. “It’s similar to a splinter that you would get underneath the skin,” says Kevin Otto, a bioengineer at the University of Florida who builds neural interfaces. They can also wear down and move around, and as a result, don’t work as well. Less commonly, they can cause more serious complications, like infection, bleeding and stroke. These risks have limited the use of DBS to patients who don’t respond to medication and BCIs to those who have lost major bodily functions.

In order for the future envisioned by the Musks and Zuckerbergs of the world to come to pass, scientists must find ways to tap into the brain in a less invasive way. One possibility: making electrodes out of living tissue instead of wire. Kacy Cullen, an associate professor of neurosurgery at the University of Pennsylvania, is trying to do just that.
Cullen uses tissue engineering to grow tiny, three-dimensional threads of brain cells that he calls “living electrodes.” Grown from stem cells and then packed into biodegradable gel tubes, these natural electrodes could be gentler in the brain, merging and connecting with living tissue rather than injuring it. He hopes they could solve some of the problems with implants used in DBS and BCIs and potentially make these treatments available to more patients.
“This is an organic interface that really allows you to speak the language of the brain — with the added benefit of it being self-renewing since it’s a living entity,” he says. Living electrodes might not merely replace traditional electrodes but also restore the “connectome,” the long-distance connections that can stretch and tear during brain injury or wither away from diseases like Parkinson’s or epilepsy.
Ultimately, a more organic BCI could also be used to better understand the brain, such as when studying people’s mental states — although he believes these applications are at least a decade away.
How to grow an electrode
To make the living electrodes, Cullen and his team start with induced pluripotent stem cells, which are generated via genetic engineering from adult cells and have the potential to turn into any type of cell in the body. They then coax the stem cells to turn into different types of neurons with long axons, the nerve fibers that carry messages between nerve cells.

Axons are critical to the complex connections that allow the brain to function. Trillions of axons crisscross the brain, making up about 60 percent of it, the part known as white matter. These tiny fibers are delicate, and if they are torn or broken, they will not regrow. “When these pathways succumb to trauma, stroke, or neurodegenerative disease, there’s really no mechanism to get them to grow back,” Cullen says. “They’re basically permanently lost.”
In his lab, axons grow into dense, three-dimensional filaments until they’re about a centimeter long and the width of a human hair. Then these long axon tracts are packaged into biodegradable polymer tubes. The result is a living electrode. One end, where the neuron cell bodies are clustered, is designed to sit on the surface of the brain while the other end can be injected into a precise spot in the brain. The gel-like tubes that the tracts are packaged in eventually dissolve in the brain, leaving behind the living axons.
The team has already implanted these bioengineered electrodes into more than 60 rats so far, where they survive for at least a month and maintain their structure. They also see evidence that the normal rat neurons and the implanted electrodes are trying to communicate with one another. Small growth projections called neurites form on the injected ends of the electrodes, and the team has also seen evidence that synapses, the specialized structures that neurons use to exchange information, are forming.
Cullen and his team were able to use the living electrodes to record brain activity in rats, suggesting that the information they collect with such a system might one day be sent to a computer and used with a BCI.
“The idea of putting in a living electrode — something that is biologically active, responsive, and alive in and of itself” opens up the possibility that a BCI or DBS system could last a lot longer, Otto says.
Better brain stimulation
Cullen thinks DBS is a more near-term application for his biological electrodes. Current stimulators deliver these shocks in a broad manner, sending electricity throughout sections of the brain. But different neurons do different things, so Cullen wants to use his living electrodes to target specific types of neurons, tailoring DBS more precisely for certain diseases.
In a paper posted to the preprint server bioRxiv earlier this year, he and his team describe how they genetically engineered certain neurons within the living electrodes to be sensitive to light. They then removed a piece of skull from rats and injected the light-sensitive electrodes into their brains. They used a device with LEDs that lays on the surface of the brain to emit light at certain wavelengths to target specific types of neurons — an approach known as optogenetics.
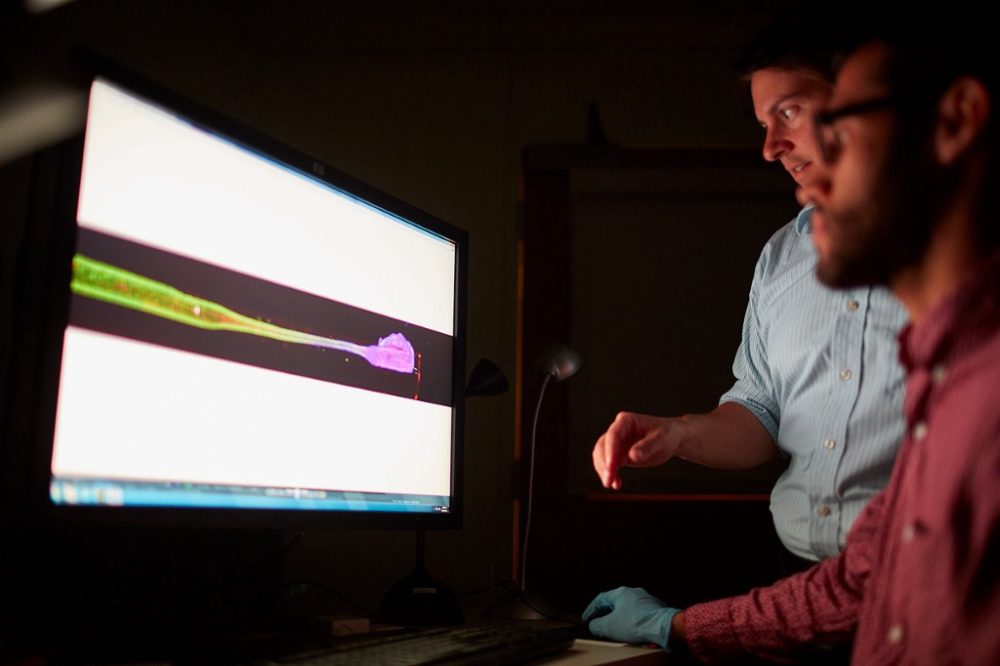
The LED device was able to stimulate only select neurons connected to the implanted axon threads, suggesting it could be used as a more specific kind of DBS. No optogenetic therapies are available yet, and the first clinical trial to test such a treatment is still underway.
Initially, a system like this might only be useful near the surface of the brain, says Kim Burchiel, a DBS surgeon at Oregon Health and Sciences University. DBS for Parkinson’s disease requires electrodes that are three to eight centimeters long, but Cullen and his team so far have only been able to grow their living electrodes out to about two centimeters. Surface brain applications might include an interface to restore sight or hearing, which are primarily processed in the cortex, the outer rind of the brain. The system might also be used with a stimulator to prevent epilepsy, since seizures start in the cortex.
“This is an organic interface that really allows you to speak the language of the brain.”
Why go to all the trouble of having this more complicated biological system when DBS has become routine for Parkinson’s? Cullen says his approach could actually restore the axon pathways that produce dopamine, the chemical that declines in the brains of people with Parkinson’s, rather than just mitigating the effects of dopamine loss. And he thinks these electrodes create new possibilities for DBS to be used in treating other conditions. “I think as the applications for conventional deep brain stimulation continue to expand our therapy could potentially get a toehold,” Cullen says. It would still require brain surgery though, so researchers will need to need to make sure the risk of opening up the skull is worth the benefit of therapy.
For now, Cullen is working on a more attainable goal. He thinks the axon threads alone could be ready for human testing in four to five years. These could be injected directly into the brain to repair brain pathways that may have succumbed to traumatic brain injury, as well as neurodegenerative diseases like Parkinson’s. Cullen has started a company, called Innervace, to commercialize this approach.
First, he’ll have to make sure the living electrodes are safe in people and aren’t rejected by the body’s immune system, which has been a hurdle in moving pluripotent stem cells into human clinical trials.
Burchiel says a biological interface between the brain and an external computer or stimulator would be an “ideal system,” but he thinks it’s something that will take a few more decades to develop. Even then, he thinks these systems will only be used for medical purposes, especially if they still require brain surgery.
“There’s a lot of appeal to this idea,” he says. “But I don’t believe we’re all going to turn into a bunch of cyborgs.”





















