Male contraceptive gels, “night-before” pills that disrupt ovulation, and the brave future of human contraception.
A few years ago, not long after it started to look like the Supreme Court could reverse Roe v. Wade, Paul Blumenthal, a professor of obstetrics and gynecology at Stanford was sitting with Erica Cahill, then a doctoral fellow in his lab, at a restaurant in Washington, D.C.’s Dupont Circle neighborhood discussing potential research projects. Knowing the statistics on how many women were repeatedly using emergency contraceptives like morning-after pills, they asked a question: Would it be possible to invent a pill a woman could take one hour before intercourse—a “night-before” pill? Now they have done it, and an early clinical study they published recently showed their new pill could disrupt ovulation for five days.
It’s no surprise that in the wake of the leaked Supreme Court Justice Alito memo, this work has taken on added significance. Many are already predicting a post-Roe-v.-Wade culture that calls for an evolution of reproductive health science and social values.
Legal experts argue that there’s nothing to suggest that in the erosion of reproductive rights, abortion is a hard stopping point. The Supreme Court’s position, though not final, could bleed into other constitutional rights like gay marriage—or even call into question a sexual privacy law based on the Griswold v. Connecticut decision, which granted married couples the right to use contraception. Hank Greely, a law professor at Stanford University and author of the book The End of Sex: And the Future of Human Reproduction says that the memo has created a situation in which all of the personal liberty cases that have been decided under the 14th Amendment could be at serious risk. The 14th Amendment, a Reconstruction-era addition to the Constitution, which was adopted in the wake of the U.S. Civil War, was designed to guarantee all people, including former slaves, due process and equal protection under the law. But the coming Supreme Court decision may undermine that.
“Alito’s saying the only way you get a liberty right is to show that specific right was ‘deeply rooted in this Nation’s history and tradition’ at the time the 14th Amendment was adopted, in 1868,” Greely says. Though he thinks it’s highly unlikely, he noted: “Contraception was not a deeply rooted right, or practice, at that time. Therefore, the logic of the Alito draft could allow states to pass laws banning even forms of contraception that cannot be claimed to be forms of abortion.”
The double threat to legal abortion and contraceptives at the state level points to the need for new definitions of body sovereignty, new routes to safe access to abortions, and new science to protect women and doctors from legal consequences. Could science really offer a solution to this unfolding social and legal problem? It wouldn’t be the first time. The history of women’s rights, in many ways, is a story of science and technology’s influence on women’s evolution towards having more freedom to control their bodies.
When the U.S. Food and Drug Administration (FDA) approved the birth control pill in 1960, it gave women a crucial boost to invest in their educations and careers, enjoy sex for the sake of it, and exercise more control over their life stories. Roe v. Wade gave them the freedom to obtain legal abortions, but it was science that provided the safest methods of terminating a pregnancy. And today, women’s economic power allows young women to pay for reproductive sciences like egg freezing and in vitro fertilization to bank their fertility and cash it in when they are older and more ready to become mothers.
These cultural shifts mean that many women living in states where abortion may soon be illegal will have to adapt and find new ways to maintain sovereignty over their own bodies. Most women of child-bearing age today have never known a world in which they’ve had this agency denied. Many will take matters into their own hands, and many will take to the internet. Crossing electronic borders could be a crucial lifeline for women who live in areas that are “maternity care and abortion deserts,” where access is limited and shrinking. Or it could be a disaster.
DIY and telemedicine abortion
“It’s going to be different than it was decades ago,” says Anna Wexler, an assistant professor of medical ethics at the University of Pennsylvania whose focus is do-it-yourself (DIY) medicine, direct-to-consumer (DTC) health products, and online patient communities. In a post-Roe world, the internet can provide women opportunities for information—and disinformation—if new laws outlaw abortion and force women to look for information and methods outside of their states. “Forums and online outlets will spring up, and women will use social media to find providers and solutions. That’s going to create a new industry to overcome the access issues. It could get dangerous.”
Since the memo leaked, Vice media has reported that Mixael Laufer, who runs the anarchist Four Thieves Vinegar Collective, released a video demonstrating how to make misoprostol tablets, a drug used to induce medical abortions, at home. These DIY recipes could be empowering in the right hands of someone who knows what they are doing, but they could obviously be fraught with the potential for life-threatening mistakes.
“I’m worried about my patients turning to unvetted sources for guidance.”
At the same time, many doctors and clinics are talking about how telemedicine could help doctors prescribe the morning-after pill over state lines. Foreseeing that health care providers may take this route, some states are trying to crack down on telemedicine. “Telemedicine will be the next battleground,” says Glenn Cohen, the director of Harvard Law School’s Petrie-Flom Center for Health Law Policy, Biotechnology, and Bioethics. “The legal question is whether these drugs that the FDA authorizes will preempt state laws, and it’s going to depend on how the state statute is written.”
There’s little comfort for me in thinking about how nuanced legal language could ensure a woman’s right to choose. Even if telemedicine provides a loophole to gain access to morning-after pills, far too many women will lack the financial means to pursue it. If women can’t afford to pay for out-of-state, out-of-network consultations, is there a way to make the consultations affordable?
For women who cannot access doctors out of state, how will they feel about their own doctors, who are bound by state laws? Will they still trust them? This question deeply concerns some doctors who fear one of the worst effects of the new laws could be to erode the trust in the doctor-patient relationship. “I’m worried about my patients turning to unvetted sources for guidance,” says Crystal Berry-Roberts, a board-certified ob-gyn who practices in Texas.
This fear may also impact women who are trying to bear children but have a miscarriage. Because there’s no way to distinguish a miscarriage or “spontaneous abortion” from an induced one, some experts are already concerned that women who have miscarriages will avoid the doctor’s office for fear of persecution by the authorities who will think she had a medical abortion. The worry is if they have excessive bleeding, or other complications, they will seek information online that is wrong or potentially illegal, and it could put their lives at risk.
“I want anyone walking through my door to feel like they can talk about what’s on their mind, so I can educate them about misinformation they might have received and help them make safe choices,” says Berry-Roberts. “That is the fundamental value in a trusting, empathetic, and open doctor-patient relationship, and I think it’s going to become more important now when it comes to women’s choice, contraception, family planning.”
At the same time, new kinds of birth control in clinical trials could become the way around any new laws and limitations of current birth control methods. But what’s coming down the pike will also ask many women and men to change their attitudes and behaviors when it comes to these potential new products.
According to the Guttmacher Institute, a research group that supports abortion rights, the rate of abortions has declined in the United States since the 1980s. In 1982, the U.S. Centers for Disease Control and Prevention (CDC) reported a rate of 29.3 abortions per 1,000 women between the ages of 15 and 44. By 2019, the last year that numbers are available, that rate had fallen to 11 per 1000, a drop due in part to an increase in birth control access and use.
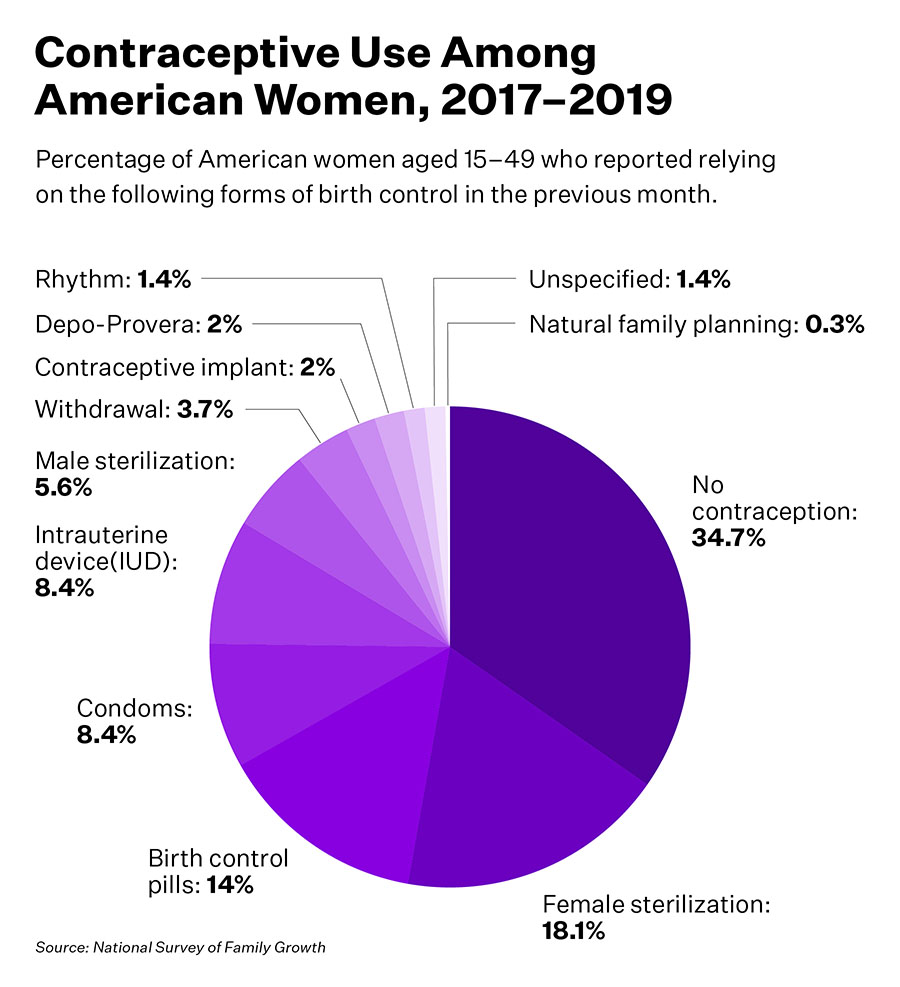
In 2018, a report by the Guttmacher Institute found that female sterilization was the most common method used, followed by the pill, male condoms, and IUDs. The two most popular methods have stayed consistent since 1982, but the notable shifts since 2002 are the increased use of long-acting reversible contraceptives such as the pill, IUDs, and implants.
The “night before” pill
There has also been an increase in the availability and use of emergency contraceptives, with a growing number of options since the first morning-after pill was approved by the U.S. Food and Drug Administration in the late 1990s. Marketed under brand names like Aftera, After Pill, Ella, My Way, Take Action, and Plan B, most of these drugs are available over the counter without a prescription. According to the CDC, one in nine sexually active women has used emergency contraception in her lifetime.While many women use it because they cannot tolerate the negative hormonal effects associated with routine oral contraceptives, there are also emerging health disparities laid bare in morning-after-pill use. Many women use emergency contraception, for instance, simply because they don’t have health insurance and can’t afford to be on the pill, says Berry-Roberts.
In a more limited future, there are two promising new methods of birth control that could skirt legal limitations and better support women. The first is ovulation disruption, or what’s now known as the “night-before pill,” which could bypass emergency contraception laws. The second is a male birth control gel, which could shift the onus of responsibility away from women to a more balanced gender dynamic.
Early trials for a new kind of emergency contraception known as the night-before pill could skirt some laws because the science would lead to ovulation disruption as opposed to emergency contraception. The “morning-after pill” works like a birth control pill but has a higher dose of levonorgestrel, a synthetic version of the hormone progestin that stops ovulation. The “night-before” pill would use different drugs to curtail ovulation earlier in the cycle.
The challenge during development was that the days before ovulation, when fertilization is most likely to occur, are the most difficult days to disrupt ovulation. Their study involved a two-cycle pill taken before intercourse that contained two drugs. The first drug, ulipristal acetate, would interfere with the process right before ovulation by blocking progesterone. The second drug, meloxicam, a COX-2 inhibitor, was meant to stop or delay ovulation by inhibiting the luteinizing hormone surge for a few days. Their study found that this drug combination disrupted ovulation in 66.7 percent of treatment cycles for five days. This is probably not effective enough to satisfy the needs of most people seeking contraception, but the pill is still in development.
“It’s early days,” says Paul Blumenthal, who led the study. “We have a conceptual framework that shows this drug combination works for ovulation disruption. We still need to study women who use the cycle of pills when they intend to get pregnant.”
If the drug does come to market eventually, it’s going to mean doctors and reproductive health educators will need to encourage a shift in how women protect their bodies from pregnancy. “They might foresee intercourse and prevent pregnancy in an on-demand fashion,” Blumenthal says. “If a woman can’t be on the pill, this could offer her an intermittent need for contraception that wouldn’t fall under the legal restrictions of the morning-after pill.” It could also reduce the cost of regular birth control pills.

Men accepting more responsibility
Another part of the social shift that will need to occur is that young men growing up and coming into their sexual and reproductive years learn to take even more responsibility for preventing unwanted pregnancies and helping women feel safe.
Currently, the NIH is supporting a countrywide clinical trial for a male contraceptive gel that contains two hormones and works in a similar way that the birth control pill works for women. In the case of men, however, the gel delivers progestin to shut down the production of sperm and testosterone to counter that effect. But unlike the pill, which works within a week, the researchers found the gel takes two to five months to become effective. “There’s a little organ above the testis called the epididymitis that I call ‘the Amazon storage facility,’” explains Mitchell Creinin, one of the lead investigators at University of California, Davis which is one of the sites of the clinical trial. “We found we can’t stop sperm production right away, so a guy will need to continuously empty the storage facility before sperm production stops, which takes two to five months.” The trial is in phase 2B, which means the researchers have identified the best dosage for a man’s sperm count to get low enough to prevent pregnancy. But the researchers still need to recruit thousands of couples to test it, which means the drug is still likely ten years or more away from becoming readily available.
“Male contraceptives would ideally need to make the penis purple and glow in the dark so women would trust it.”
In the meantime, it could allow health educators to support a new message that men can partake in birth control beyond condoms and vasectomies. “I’ve learned in talking with many couples that male contraceptives would ideally need to make the penis purple and glow in the dark so women would trust it,” Creinin says. This may be because for so long, women have primarily faced the implications of getting pregnant, and therefore have learned to look out for themselves. At the same time, Creinin says that in talking with every couple in this study, he saw that men wanted to be a bigger part of those implications, not only for themselves to avoid causing a pregnancy but to take the weight off their partner. “These new methods are going to change how we talk about sexual health, how we teach about it, and how kids from a young age will grow up to learn responsibility in a shared dynamic around sex,” Creinin says.
I nodded when I heard Creinin say this because it hit so close to home. I conceived my nine-year-old son in the privacy of my own home with the help of reproductive science because I believed in choice and sovereignty over my body. I’ve tried to raise him to have a deep respect for women’s choices and sovereignty over their bodies, and I have tried to instill in him the understanding that being a young man today does not mean taking power away from women but having agency in standing equally by their side. In recent days, those lessons have been coming like a firehose.
“Stay out of my pussy!” shouted the young teen girl protesting outside our local high school as I drove my son home from school last week. “What’s a pussy?” he asked, inevitably, and I told him that women were angry because the federal government might take away what we thought was a fundamental freedom.
I’m now terrified of him growing up in this new world of both scientific and legal limitations, distrust, and bias against women and LBGTQ+ families. But the new sense of shared responsibility around sex really gives me hope.
The next time we drive past a “stay out of my pussy” sign, I might suggest that he roll down the window and scream, “You go girl!”

























