How I hacked my diet using a continuous blood-glucose monitor.
Most health recommendations are one-size-fits-all: Do this, don’t do that, based on large studies that assume you’ll fit somewhere in the middle. This is particularly true with diet and nutritional advice, as different foods are considered good or bad based on how they affect most people. But you’re not most people — you’re you. Happily, recent advances in genomics, microbiome testing, and machine learning promise far more personalized health insights.
Now there’s a powerful, cost-effective tool for making dietary decisions based on your personal body chemistry nearly in real time: a continuous blood-glucose monitor.
Designed to help people cope with diabetes, such devices in the past have been expensive and required a needle to draw blood. But the U.S. Food and Drug Administration in 2017 approved Abbott’s FreeStyle Libre, a button-sized sensor patch you stick painlessly on your arm that measures blood glucose once a minute. In November, the agency approved LibreLink, an iPhone app that displays the readings without additional hardware.
That move effectively transformed this medical device into a consumer product.
I gave the patch-and-app system an intensive workout, and I was amazed by what I learned about how my body reacts to the food I eat. For instance, from now on I’ll eat pasta only with olive oil or animal fat, and please don’t offer me wine with dinner.
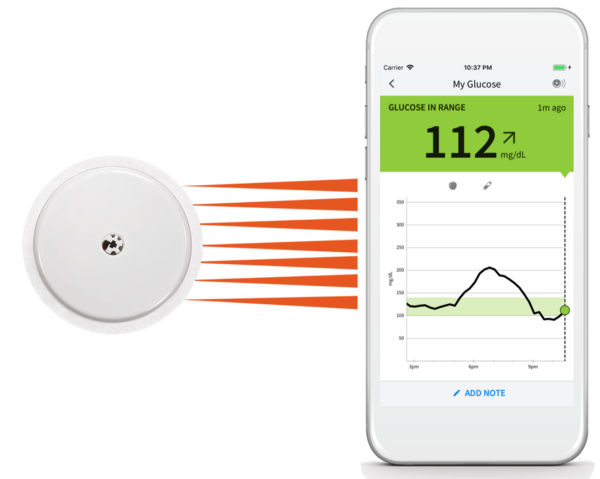
The blood-sugar equation
Many factors determine whether or not a particular food is good for you, but one simple measure stands apart: blood glucose. Food gives you energy because your body turns it into glucose, a type of sugar that powers every living thing. Too little, and your cells run out of energy, leaving you tired and hungry. Too much, and it damages cells and can even kill you.
Your body is programmed to regulate blood glucose automatically to Goldilocks levels: not too high, not too low. In healthy people, that typically means between 100 and 140 milligrams of glucose per deciliter of blood (mg/dL). Nonetheless, some foods can cause an unhealthy spike — something to avoid, if possible. General guidelines work for most people, most of the time. But we’re all different, and it’s a good bet some foods make your blood-glucose levels go haywire.
At this point, the technology is cheap and easy enough that even non-diabetics can benefit.
Too many spikes and your body can become resistant to the glucose-regulating hormone insulin. If that happens, you’re likely to develop diabetes, a condition that requires you to monitor your glucose levels carefully day and night, alternately eating or injecting insulin if things get out of control.
Because many millions of people suffer from this condition, scientists and engineers keep developing cheaper and less-intrusive ways to measure blood glucose. At this point, the technology is cheap and easy enough that even non-diabetics can benefit.
The continuous glucose monitor goes mainstream
The FreeStyle Libre is available in the U.S. by prescription, which many doctors will write if you point them to the FreeStyle Libre healthcare provider website, which explains safety and usage information. It costs about $80 for two sensors that last two weeks each — a month’s supply. If you don’t have an iPhone 7 or later, you’ll also need a $200 reader. In Canada and many other countries, you can buy the sensor at your local pharmacy without a prescription.
The patch is easy to apply. It comes with a waterproof adhesive strong enough to wear in the shower or swimming. It comes with a plastic gadget you press against your arm with just enough force to push a tiny, hairlike filament into your skin. It looks like a needle, but it’s not, and it doesn’t feel like one. No blood, no pain; just a bit of one-time pressure. After an hour’s wait for the device to calibrate itself, you can run an iPhone over the patch and see your glucose level.
How accurate is it? The gold standard is the traditional blood glucose meter, a device that requires a tiny drop of blood from a needle prick. To test the accuracy of my much simpler, needle-less continuous glucose monitor, I drank a blueberry-banana smoothie and after about 45 minutes, I pricked my finger and placed a drop of blood into two separate meters. One gave a reading of 111, the other showed 113 — about the same.
A reading at the same time with the FreeStyle Libre gave a wildly different number: 144. But the arm sensor is measuring the interstitial fluid under the skin, which isn’t quite as fast to respond to glucose changes as the blood. I waited another ten minutes, and the Libre showed 111.
What my glucose levels told me
In previous proto.life reviews, I wrote about microbiome genetic sequencing tests from DayTwo and Viome that offer custom diet advice based on research that shows a relationship between gut bacteria and blood glucose levels. Those tests predicted how well my body would respond to particular foods.
The FreeStyle Libre system showed my actual glucose levels. Its readings lined up pretty well with the microbiome tests’ predictions. For example, the $300 DayTwo test said instant ramen is really bad for me. Yeah, if you read the label, it’s obvious this ain’t health food.
But the FreeStyle Libre made the problem obvious. It registered a huge spike just minutes after eating a bowl. In fact, I have yet to see a higher reading. Even a sugary donut didn’t produce the glucose spike of packaged ramen.
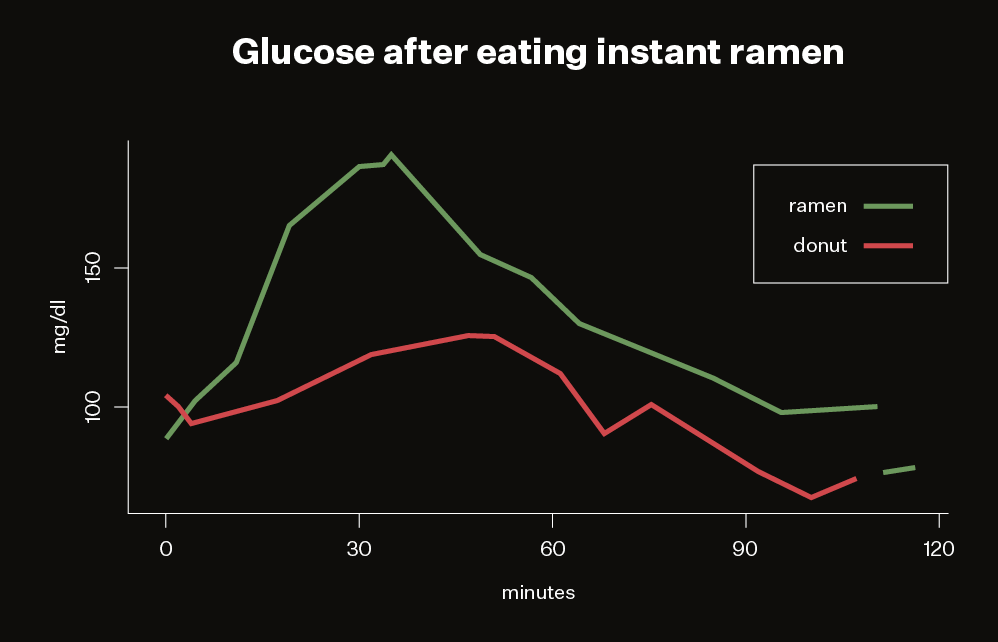
But the patch-and-app combo really came into its own when I experimented with combining foods to reduce such spikes. For example, despite all the advice you may hear about the health benefits of oatmeal, even a single bowl produced terrible readings. Adding cinnamon, which research supposedly shows can moderate glucose, did nothing for me and may have made it worse. However, adding a little milk or, better yet, butter, tamed the spike.
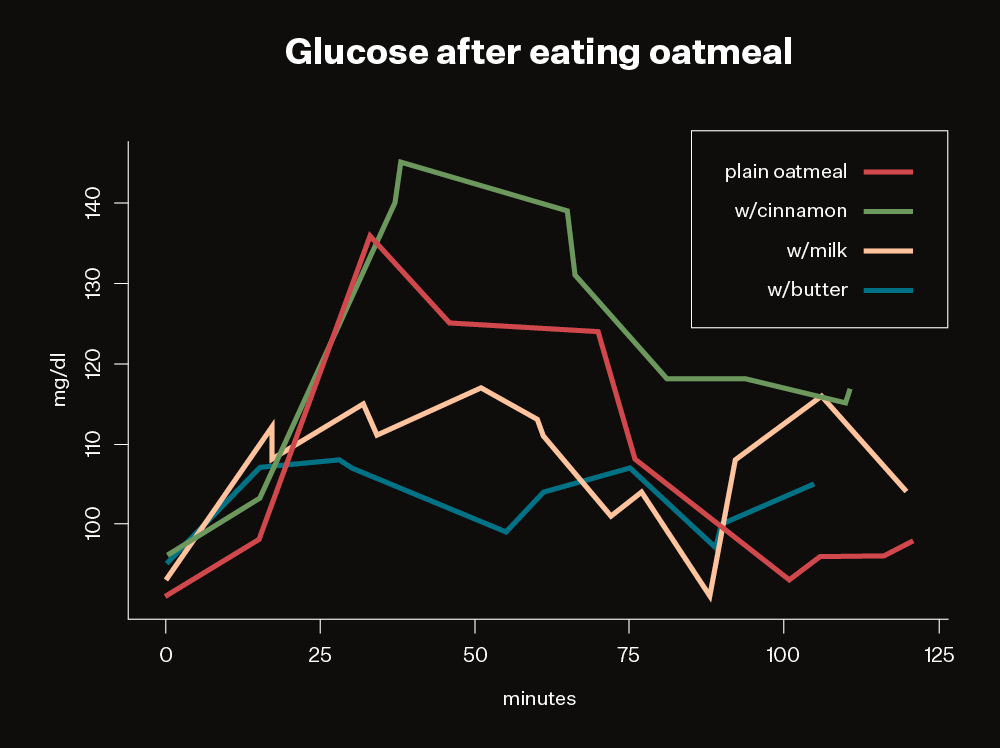
Most discussions of blood glucose warn that starchy foods like potatoes are bad. My results confirmed that for me. But some people say potatoes are okay if they’re reheated, since the process of heating, cooling, and reheating supposedly transforms the starch in a way that gut bacteria like, which in turn keeps glucose levels stable.
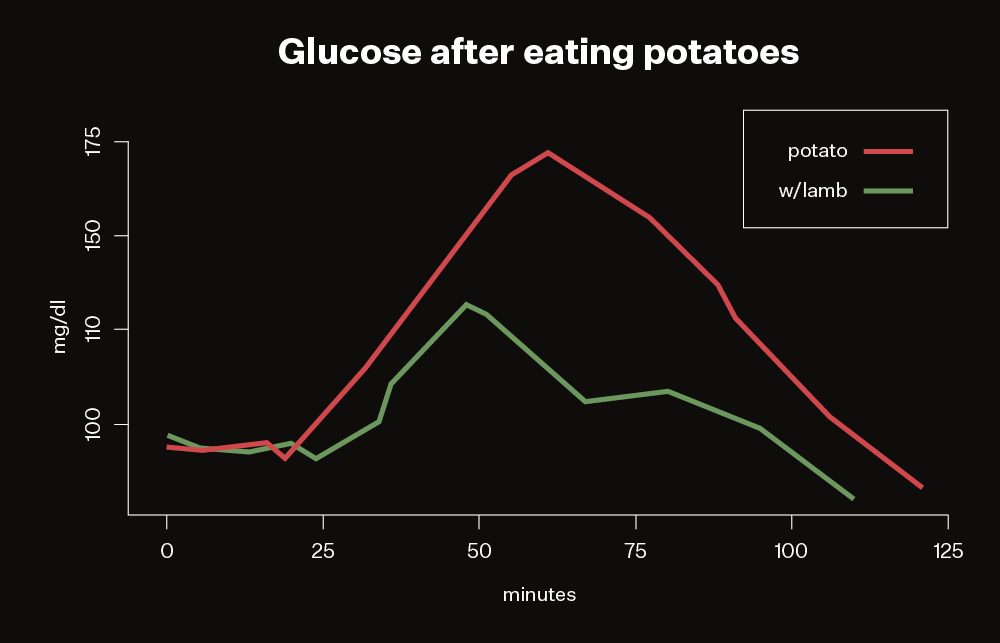
Sadly, that doesn’t appear to work for me. Reheated potatoes caused a large spike. On the other hand, eating a regular boiled potato with fatty lamb and gravy kept the glucose rise to reasonable levels. In other words, it looks like I can eat potatoes as long as they’re served with meat.
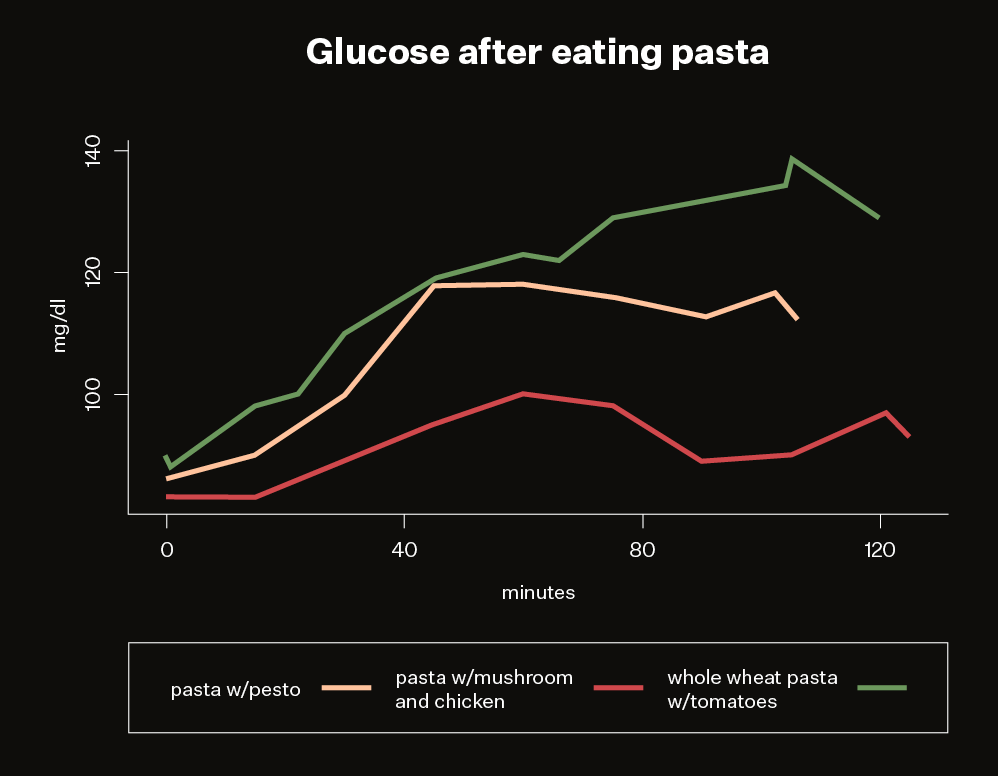
Then there’s pasta which, along with bread, is often considered a glucose-raising carbohydrate. But different pastas had different effects for me, and some raised my blood glucose much higher than others. Fettuccine didn’t produce much of a glucose rise — as long as I smothered it in fatty pesto or mushroom chicken. But ordinary tomato sauce, even on whole wheat pasta, pushed my glucose higher.
What about alcohol? A glass of wine with a meal caused a precipitous drop in my blood glucose. At first, I thought that was a good thing. The drop was so dramatic that I even gave myself permission to indulge in a sugary dessert, thinking perhaps I’d discovered a neat trick to keep glucose in check.
Alas, upon reading the literature, I discovered the opposite: Glucose levels drop because the alcohol confuses the body into making too much insulin, interrupting other important functions in order to expel it.
For most type 1 diabetics, research shows, a glass of wine at dinner doesn’t affect glucose levels the same night, but results in significantly lower levels the following morning, apparently due to reduced growth hormone secretion during sleep. Not only that, but alcohol blocks production of glucose in the liver, which keeps emergency stores if your glucose goes too low.
Bottom line: Monitoring my blood glucose persuaded me to treat alcohol as an indulgence, a rare treat to enjoy now and then on strictly social occasions, but definitely not on a daily or even weekly basis. Apparently, it’s just not good for me.
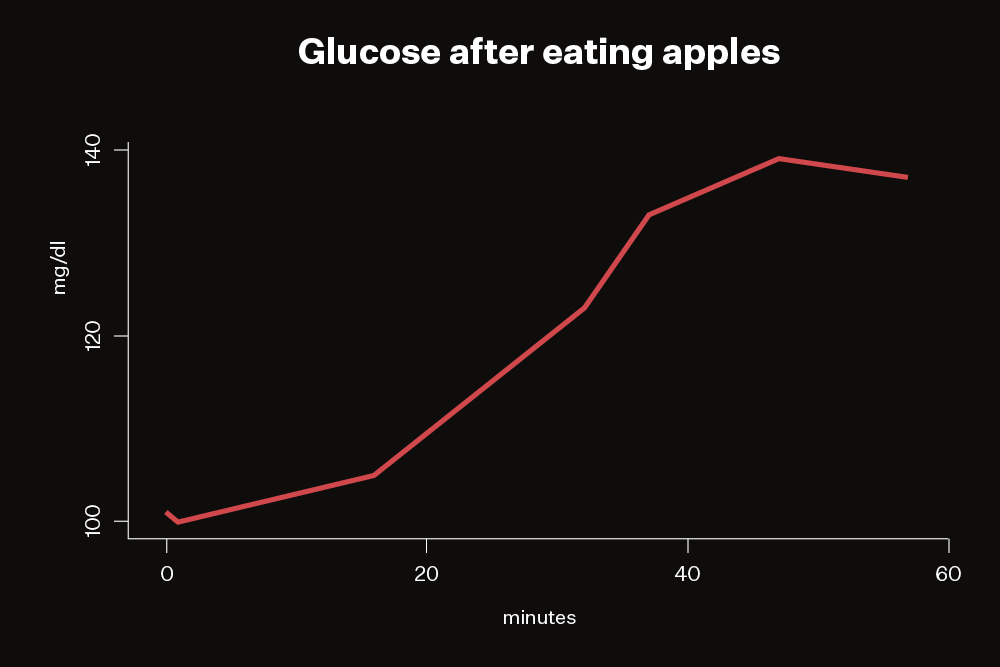
I said in my earlier review that DayTwo and Viome disagreed about whether apples are good for me. What did the glucose monitor say?
To find out, I ate a medium-sized organic apple on an empty stomach. Sure enough, as DayTwo predicted, the apple spiked my glucose. As with oatmeal and pasta, maybe I can moderate the spike by combining the apples with something else. Fortunately, thanks to the immediate feedback from my continuous glucose monitor, it’s easy to experiment with different combinations to learn more about what works — and doesn’t work — for me.
And that may be the greatest benefit of these new self-tracking technologies. By giving me immediate, actionable insight into how food affects me, I’m able to adjust in time to have an impact. Wearing the FreeStyle Libre, even for a few weeks, let me taste a future where we can all learn how our bodies are unique and how to optimize their performance.



















